Ultrasound Case Study
Trigger Finger..or was it?
Stuart Wildman, Extended Scope Physiotherapist and MSK Sonographer
This patient was in their late teens and was referred for a ‘trigger finger, please inject’, I thought it made an interesting case so have written it up here for discussion. Initial thoughts were that this would be a fairly straight forward referral as trigger finger is often a pleasing condition to treat with good response rates to a local steroid injection. I then saw the patients age being in the late teens, and immediately you become fairly sure that it isn’t a trigger finger, or at least an unusual presentation in someone of that age. The patient reported a gradually increasing awareness of a lump in her hand, with no triggering of the finger. It was tender to touch and they felt it was becoming progressively larger. There was no pain at rest. There was no history of trauma, and no locking.
Primary trigger finger occurs most commonly in the middle fifth to sixth decades of life and up to 6 times more frequently in women than men (Makkouk et al, 2008). The lifetime risk of trigger finger development is between 2 and 3%, but increases to up to 10% in diabetics (Stahl et al, 1997). The rate of occurence in diabetics is associated with actual duration of the disease, not with level of glycemic control (Chammas et al, 1995) . There also appears to be an increased chance of developing trigger finger in patients with carpal tunnel syndrome, de Quervain’s disease, hypothyroidism, rheumatoid arthritis, renal disease, and amyloidosis . The ring finger is often the most commonly affected, followed by the thumb (trigger thumb), long, index, and small fingers in patients with multiple trigger digits.
With trigger finger, inflammation and hypertrophy of the retinacular sheath progressively restricts the motion of the flexor tendon (Newport et al, 1990). This sheath normally forms a pulley system comprised of a series of annular and cruciform pulleys in each digit that serve to maximize the flexor tendon’s force production and efficiency of motion(Newport et al, 1990). The first annular pulley (A1) at the metacarpal head is by far the most often affected pulley in trigger finger, though cases of triggering have been reported at the second and third annular pulleys (A2 and A3, respectively), as well as the palmar aponeurosis.
The patients medical history was otherwise unremarkable, and of note she was not diabetic. She was not taking any medication, and had a healthy lifestyle participating in sport and studying at college.
On observation and palpation, there was large area of thickening proximal to the 2nd MCPJ, which felt hard to touch. There was no redness or visible swelling. There was full range of movement of all associated joints in the area. Resisted tests were unremarkable, with no pain provocation. As previously mentioned, the patient was not able to demonstrate any locking and could not recall any episodes of this.
With the use of Musculoskeletal Ultrasound , I further investigated and encountered a large multi-lobulated lesion in the region of the 2nd metacarpal with no clear vascularity and was not compressible. At that point, this was clearly not an issue for me as a Extended Scope Physiotherapist to further manage and so I liased promptly with the GP and the patient was referred urgently for further imaging within the Radiology department at the local hospital. The use of ultrasound here did facilitate the management, in that I was able to confirm that this was not a trigger finger and that the pathology was potentially sinister and needed urgent review.
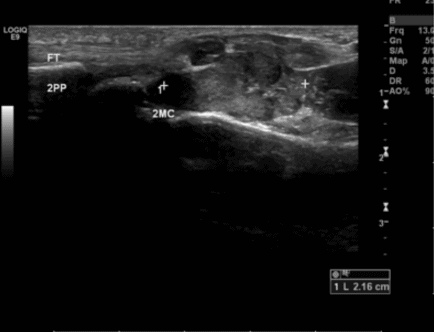
The patient then went on to have an urgent ultrasound, the images of which are below in both the transverse and longitudinal view. There was also no vascularity demonstrated.
The report of the formal ultrasound was…There is a lobulated 2cm soft tissue swelling with no significant increased vascularity, overlying the radial aspect of second metacarpal. It deflects the flexor tendons of the index finger. It is closely applied to the underlying bone but the cortex is intact. Appearance may represent a giant cell tumour of the flexor tendon sheath but other soft tissue tumour cannot be excluded. An MRI has been urgently arranged.
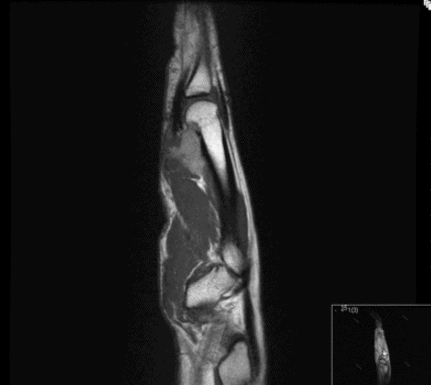
The report for the MRI was ‘ The lesion seen on ultrasound is demonstrated as a lobulated soft tissue lesion measuring about 2.2cm in diameter which is isointense with muscle on T1 sequences and slightly hyperintense on T2 weighted sentences. It appears to arise from the epiphyseal region of the distal end of the second metatarsal. There is a slightly scalloped appearance of the volar cortex at this level. It is closely applied to the distal metatarsal. It extends superficially displacing the flexor tendon slightly. Post injection of contrast there is a diffuse homogenous moderate enhancement. Lobulated soft tissue mass which appears to arise from the metacarpal. Appearances suggest a giant cell tumour.
This patient is now planned to go for surgery to excise the tumour.
This provided an interesting case on the differential diagnosis for trigger finger. Without the use of ultrasound you would hope that an MSK clinician would have picked up the unusual nature of the presentation, however MSK Ultrasound in clinic did facilitate the management.
Giant Cell Tumours are one of the most common soft tissue tumours of the hand (Middleton, 2004). Here is a free full text article by Wang et al (2007) from the great resource that is The Journal of Ultrasound Medicine. This provides a thorough overview of the presentation and the use of sonography. A further article by the previously referenced Middleton (2004) is also free access and can be found here.
An overview of ultrasonography and the diagnosis of soft tissue tumours..
References
Chammas M, Bousquet P, Renard E, et al. Dupuytren’s disease, carpal tunnel syndrome, trigger finger, and diabetes mellitus. J Hand Surg [Am] 1995;20:109–14.
Stahl S, Kanter Y, Karnielli E. Outcome of trigger finger treatment in diabetes. J Diabetes Complicat.1997;11:287–90.
Newport ML, Lane LB, Stuchin SA. Treatment of trigger finger by steroid injection. J Hand Surg [Am]1990;15:748–50.


0 Comments